Pressure or “ball-like” fullness when sitting
Often worse on firm chairs, in cars, or after prolonged sitting; may ease when standing, walking, or lying down, then returns quickly with re-loading.
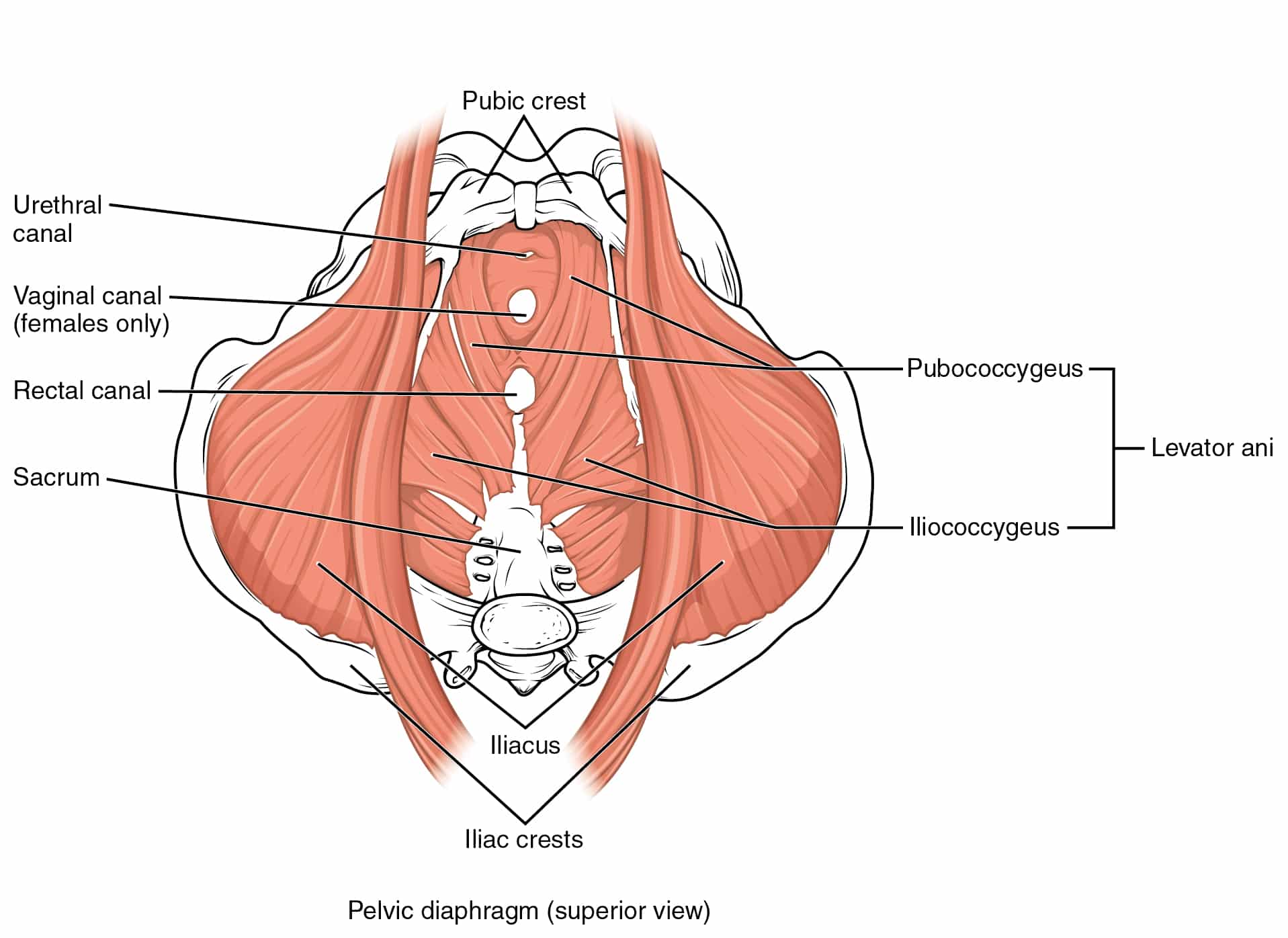
“Feeling like sitting on a ball” is a recognizable symptom pattern, usually described as a localized fullness or pressure at the perineum, tailbone region, or deep rectal/vaginal area. Functionally, it is often linked to protective pelvic floor muscle overactivity (hypertonia), irritability of the levator ani complex, and a sensitized interface between muscle, fascia, and nearby nerves.
When the pelvic floor stays “on,” small loads become big signals. Sitting compresses already sensitive tissues and can amplify neural input from pudendal and sacral nerve branches. The result is sitting intolerance, positional pain, and a feeling of swelling or a foreign object even when there is no true mass.
In clinic, we treat this as a capacity problem rather than a purely structural one: reduce tissue irritability, normalize pelvic floor coordination, and rebuild sitting tolerance with a phased desensitization plan tied to function-first goals.
Standard care often looks for a single diagnosis that shows up clearly on imaging or lab work. When those tests are unrevealing, treatment may default to medication trials, generalized pelvic floor strengthening, or reassurance. These approaches can miss the gap in care: functional drivers such as myofascial trigger points, protective guarding, nerve mechanosensitivity, and load intolerance that do not reliably appear on MRI or ultrasound.
Similarly, structural interventions may not address the pain generator if the dominant issue is hypertonic muscle behavior and sensitized peripheral input. Without hands-on mapping of tissue response and a progression plan for sitting exposure, symptoms can remain unpredictable.
Not necessarily. The sensation can be produced by hypertonic pelvic floor tissue, localized trigger points, or nerve sensitivity without a true mass. Because medical causes are possible, it is appropriate to see a physician for pelvic/rectal evaluation, especially if symptoms are new, progressive, or associated with bleeding.
Seek urgent medical care for rectal or vaginal bleeding, fever, acute severe pelvic or abdominal pain, new urinary retention, sudden bowel changes (especially new incontinence or inability to pass stool/gas), or rapidly worsening symptoms. These findings require medical evaluation beyond functional treatment.
If the main issue is elevated tone with focal trigger points, the limiting factor may be tissue irritability and neural sensitivity rather than flexibility alone. Assessment-driven dry needling and acupuncture can help reduce myofascial guarding and improve the pelvic floor’s ability to change tone, which can make later strengthening or coordination work more effective.
It depends on chronicity, sensitivity, and how restricted sitting is. Many patients start with a short block of visits to reduce irritability and establish a trigger map, then taper as tolerance improves. Your plan is adjusted based on objective changes like sitting time, flare recovery, and reproducible exam findings.
Not always. Some cases respond well to external and adjacent structure treatment (hip rotators, sacral region, abdominal wall) plus coordination training. If internal assessment or treatment is clinically relevant, it is discussed beforehand and performed only with informed consent and clear rationale.
They can, especially when pelvic floor tone is already elevated or sitting pressure is a primary trigger. The goal is not blanket avoidance. We identify the specific load variable that provokes symptoms (seat pressure, breath-holding, intensity, duration) and rebuild exposure in a phased way that protects progress.
While acupuncture does not hurt, you may feel a “de qi” sensation—a deep, dull ache or heaviness at the point of insertion when the thin needles stimulate the connective tissue and nervous system. This is a natural and effective part of the acupuncture treatment, indicating that the acupuncture point is being activated. The patient is always in control, and most find these sensations well-tolerated or enjoyable. Schedule an Appointment or Free Phone Consultation
Most people feel a quick twitch or brief pinch during a dry needling session as the needle interacts with myofascial trigger points or muscle fibers in the affected area, but it’s usually well tolerated and any muscle soreness fades quickly—many patients say the relief is worth it. Schedule an Appointment or Free Phone Consultation
The benefits of dry needling are numerous, especially for pain management. This treatment method effectively targets myofascial trigger points within tight muscles, helping to release muscle tension, improve muscle function and range of motion, and stimulate the body’s natural healing process. It can be particularly effective for soft tissue injuries, overuse injuries, and chronic pain conditions like myofascial pain syndrome by addressing the root causes of discomfort in specific areas of the body. Many find it helps accelerate recovery time from a muscle strain or injury. Schedule an Appointment or Free Phone Consultation
This varies based on the patient’s medical history and condition, but many patients see results over time depending on their condition. Pain-related conditions often initially have quick results, though recovery time can differ. This will be discussed during the initial consultation. Schedule an Appointment or Free Phone Consultation
Yes, acupuncture and dry needling complement most standard medical treatments, including physical therapy treatments or chiropractic care, and Dr. Barber can collaborate with other healthcare providers as needed. Schedule an Appointment or Free Phone Consultation
The first acupuncture appointment or dry needling session includes a detailed initial consultation where Dr. Barber reviews the medical history, discusses specific needs and musculoskeletal condition, performs an assessment, and provides the first personalized treatment option. Schedule an Appointment or Free Phone Consultation
Yes, I treat adults, teens, and children (though I do not specialize in infants or toddlers). I’m experienced in working with sensitive issues and strive to create a welcoming, inclusive space for all patients, including those in the LGBTQIA+ community. For pelvic floor patients who are post-operative following gender-affirming surgery, I do not have specialized training in this area, but if you’re able to provide detailed surgical notes, I’m open to collaborating and finding safe, supportive treatment solutions together. Schedule an Appointment or Free Phone Consultation
Yes — we are an out-of-network provider and can submit to most PPO insurance plans. While we are not contracted with any insurance companies, we want to make it as easy as possible for you to use your benefits when available.
We do not participate with Medicare or Medicaid, including Part C out-of-network coverage.
✔ Claims Submitted on Your Behalf
We now submit out-of-network claims directly to your insurance company as a courtesy to help streamline your reimbursement process. Payment is due at the time of service, and reimbursement (if any) is sent directly to you based on your plan’s coverage.
✔ Complimentary Insurance Verification
We offer free verification of your out-of-network benefits before your first visit so you know what to expect. Please note that benefit verification is not a guarantee of coverage or payment. Click Here for our verification form.
✔ FSA & HSA Payments Accepted
We accept Flexible Spending Accounts (FSA) and Health Savings Accounts (HSA) for all eligible services.
✔ For Your Records: CPT Codes We Commonly Use
If you prefer to call your insurer yourself, you can ask about out-of-network acupuncture benefits using the following commonly billed CPT codes:
99202 – New patient evaluation (approx. 20 min)
99203 – New patient evaluation (approx. 30 min)
97810 – Acupuncture, initial 15 min (no electrical stimulation)
97811 – Acupuncture, each additional 15 min (no electrical stimulation)
97813 – Acupuncture, initial 15 min (with electrical stimulation)
97814 – Acupuncture, each additional 15 min (with electrical stimulation)
20560 – Dry needling, 1–2 muscles
20561 – Dry needling, 3+ muscles
97140 – Manual therapy (e.g., myofascial release, trigger point therapy)
We do not follow up with insurance companies after claim submission, and we cannot guarantee reimbursement. However, we are happy to provide treatment notes or documentation upon request to support your claim if needed.
We do not participate with Medicare or Medicaid, including Part C out-of-network coverage. Medicaid Advantage may provide some reimbursement.
If you have secondary out-of-network coverage, this may be an option for reimbursement.
Yes, I offer a free phone-based Q&A session to see if we are the right fit to work together. This is an opportunity to address your questions and ensure that my approach aligns with your health goals. You may book your Q&A session here: Schedule an Appointment or Free Phone Consultation
Most people feel a quick muscle movement (that local twitch response we talked about), a brief cramp, or a dull ache. Some spots might be a bit more sensitive, but overall, it’s usually not too uncomfortable. Dr. Barber is very careful to make the effective treatment as beneficial as possible with minimal discomfort.
How many treatment sessions you’ll need depends on your specific problem, how long you’ve had it, and your general health. Some issues get better after just a few visits, but long-term or tricky conditions might need more treatment. Dr. Barber will talk with you about your personal treatment plan during your first visit. The effectiveness of dry needling can vary, but many find it an effective treatment for trigger point therapy.
When done by a trained expert like Dr. Barber, who is among the licensed acupuncturists also skilled in this Western medicine technique, dry needling is very safe. We always use clean, new needles for each patient and follow strict healthcare safety rules. Dr. Barber will ask about your health history to make sure it’s safe for you, especially if you take blood thinners or have a weakened immune system (compromised immune systems).
It’s a good idea to have eaten something before you come. Wear comfy, loose clothes so Dr. Barber can easily reach the area that needs treatment. And please, bring any questions you have about your condition or the dry needling treatment! Schedule an Appointment or Free Phone Consultation
Generally, no. For most people and most conditions, expertly performed dry needling is highly effective without ultrasound guidance. While ultrasound can be a helpful tool in rare, very specific situations, research suggests it doesn’t necessarily make dry needling treatment more effective for common trigger points.³ Dr. Barber relies on his extensive training, precise anatomical knowledge, and years of experience to deliver safe and effective treatment. Some clinics may push for routine ultrasound guidance, but this can often lead to unnecessary costs. For a more detailed explanation, you can read Dr. Barber’s article: Do You Need Ultrasound Guided Dry Needling?
Pelvic floor dry needling is a targeted treatment using thin filiform needles to release trigger points and muscle tension in the pelvic floor. It may help reduce pain, improve muscle function, and restore normal movement patterns.
Most patients feel a brief muscle twitch or cramp-like sensation during treatment. Discomfort is usually short-lived and often followed by a feeling of release or relief.
We maintain your comfort and privacy while working within your boundaries. Depending on the location being treated, undressing may be needed, but always with appropriate draping/covering. Internal examination and techniques are not performed or required.
Yes. I treat adults of all genders and identities. I provide a welcoming, inclusive environment. For post-operative gender-affirming care involving the pelvic floor, please bring surgical notes so we can assess appropriateness and safety together as each patient is very unique.
The number of treatments varies depending on the condition, its severity, and your response. Many patients notice improvement within 3–6 sessions, though complex cases may require longer-term care.
Yes, when performed by a trained, licensed provider with experience in pelvic anatomy. All needles are sterile and single-use. The procedure is precise and tailored to your needs and comfort level.
In NY State the only providers legally allowed to perform dry needling are Medical Doctors (MD), Doctors of Osteopathic Medicine (DO), Nurse Practitioners (NP), Physician Assistants (PA), and Acupuncturists (LAc). It is forbidden by the State Board for Chiropractors (DC) and Physical Therapists (PTs) to perform dry needling regardless of their training. For your safety, please choose a provider that is both properly trained and legally allowed to perform the technique.
Most pelvic floor conditions do benefit from dry needling, especially those involving muscle tension, trigger points, or nerve irritation. However, I require all pelvic floor patients to have an active diagnosis from a qualified medical provider or pelvic floor physical therapist. This is because dry needling is often just one part of the overall treatment strategy—it works best when integrated with a broader care plan that may include physical therapy, medical management, or other interventions. My goal is to ensure that dry needling is applied safely and appropriately as part of a comprehensive approach tailored to your specific diagnosis.

